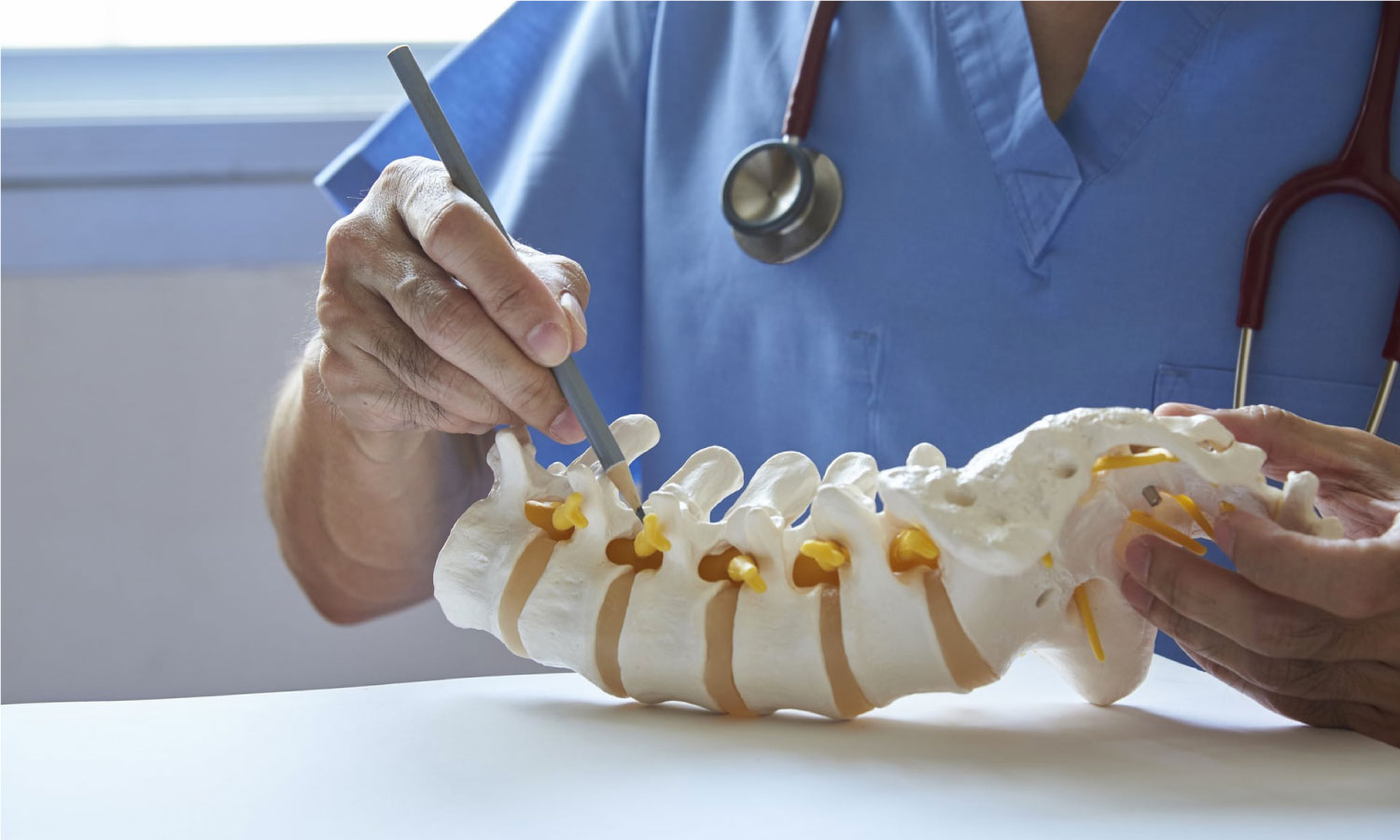
Spine problems, causes and treatment
The importance of the spine lies in protecting and protecting the spinal cord, rib cage, and nerves. The vertebrae can provide the necessary support for the moving structure; It also provides protection for the nervous tissue that runs from the brain to the spine from injury. Spinal diseases vary according to the location of the injury and its symptoms. On this basis, the doctor sets a mechanism for treatment that begins with primary and physical treatments, and the last stage is surgery, which has witnessed an amazing development in recent years, which has led to some operations performed by local anesthesia and some are performed by endoscopy.
Before discussing the problems, it is important to clarify the composition of the spine and its functions in the body. The spine consists of platform-like discs that act as cushions between the vertebral bodies, reducing the impact of movement on the spine. Because of their location between the vertebrae, the discs are sometimes referred to as intervertebral discs.
Degenerative spinal diseases
When one of the spinal discs loses its strength, degenerative disc disease occurs. Disc disease is the emergence of alterations in the spinal discs, resulting in significant discomfort. This condition occurs when the intervertebral discs dehydrate and lose their fluid content, causing friction between the vertebrae and reducing their ability to absorb shocks.
The onset of the disease is straightforward, but it worsens with age, causing rupture and erosion as the body’s cartilage weakens and becomes brittle; Because each of the discs and joints that stack the vertebrae is partially composed of cartilage, these areas are susceptible to damage and rupture; these areas are referred to as degenerative changes, and along with the gradual deterioration of the discs located between the vertebrae. Spinal discs are made up of a soft inner core and a tough outer wall. These discs deteriorate as we age, resulting in degenerative disc disease.
Dehydration is one of these changes. These discs are largely water-filled at birth, but as they age, they lose water and become thinner. Flat, thin discs are incapable of absorbing shock, and their ability to provide protection between the vertebrae decreases as they lose water, resulting in spinal issues and discomfort.
Erosion is another type of change that can occur to the discs. Daily movements and secondary injuries may produce minute tears in the outer wall containing the nerves; any tear near the nerves causes discomfort. When the outer wall fractures, the soft inner disk’s center can be forced through these cracks. A bulging disc or one that has fallen out of place is referred to as a slipped disc. It may also have an effect on adjacent nerves.
The symptoms vary according to the location of the weak or damaged disc; the patient’s symptoms are severe back and neck pain. The most common symptoms of disc pain include pain in the lower back, buttocks, or upper thighs that lasts for days or even months and changes in intensity depending on the patient’s effort. However, this pain worsens when sitting and improves when moving or walking; it also worsens when bending and improves when shifting the body’s position or lying down. Degenerative disc disease can occasionally result in numbness in an arm or leg. Additionally, it may result in weak leg muscles, indicating that damage to the spinal discs may have an effect on the nerves near the spine.
After walking and exercising, the patient may feel reduced pain. Additionally, this condition might cause weak leg muscles and numbness in the arms or legs. Advanced stages of degenerative disc degeneration can result in back osteoporosis. Due to the absence of discs between the vertebrae in this form of osteoporosis, the vertebrae rub against each other, causing back discomfort and stiffness and severely restricting the types of activities that the patient may comfortably perform.
Spinal disc herniation
A herniated disc, or disc pain, occurs when the disc’s nucleus pulposus ruptures and protrudes through its outer fibrous ring. The disc between the fourth and fifth lumbar vertebrae in the lower back is the most likely to herniate. A herniated disc occurs when the disc becomes weak due to pressure or other factors. It ruptures, exposing the disc’s interior material to the outside, or it bulges. Herniated discs can occur in any part of the spine, from the neck to the lower back, but they are most frequently found in the lower back. This slide irritates the nerves near, resulting in severe pain, numbness, and weakness at the damage area.
This health condition results in severe pain in the back, and the spine includes a complex network of nerves and blood vessels, and if the herniated disc causes pressure on the nerves or nearby muscles, the patient may suffer from some other additional symptoms, including severe pain in the legs; In the event of a herniated disc in the lower back, the pain is often concentrated in the buttocks, thigh, and legs, and the pain can extend to parts of the foot.
Additionally, the patient may suffer numbness and tingling along the nerve that is compressed by the herniated disc, as well as weakness in the muscles serviced by the herniated discs nerves.
It should be noted that the symptoms of a herniated disc are not related to back pain, but rather appear as problems in the extremities and differ according to the type of slip, particularly because it is classified into two types: the first is a cervical disc herniation, which occurs in the upper vertebrae and manifests as pain and numbness in the upper extremities and numbness in the arms, and the second is a lumbar disc herniation, which occurs in the lower.
The treatment of a herniated disc does not depend on surgery in all cases, but rather depends on the degree of the herniated disc, which is divided into 5 basic degrees:
- The first degree entails a slight deviation of the cartilage so that the nerve is not significantly harmed. When standing or sitting for long periods of time, the patient experiences slight numbness, and his treatment consists solely of exercises to strengthen the back muscles.
- The second degree, in which the patient has weakness and stretching of the fibrous ring surrounding the cartilage, but it has not yet been cut, so treatment is limited to therapeutic back exercises.
- The third degree: a cut has occurred in the fibrous ring surrounding the cartilage, but it has not yet come out, and its treatment depends on the doctor’s discretion and the degree of the cut.
- The fibrous ring has been cut and the cartilage has been removed and compressed on the nerve when the patient reaches the fourth degree, and the majority of the treatment is surgery or endoscopy, cartilage excision, and artificial cartilage implantation.
- Because the cartilage is completely out of the fibrous ring and suffocates in the channel in which the nerve runs, the fifth degree is one of the most difficult stages to treat because the pain is unbearable in the back and limbs, and the patient is unable to move, and the basic treatment is to remove the cartilage. It’s a surgical procedure.
Spinal stenosis
It is a narrowing of the spinal canal within the spine that leads to pressure on the spinal cord and the nerves that travel through the spine to the feet and legs. This disease usually occurs in the lower back or in the neck.
This problem occurs when the spaces between the bones that make up the vertebrae narrow, causing pressure on those bones and on the nerves that extend from the spine to the arms and legs, and this occurs most often in the lower back or neck,
There are several reasons that lead to infection, including tumors in the spine, overgrowth of bones, spinal injuries, and others. Symptoms of this disease include numbness or tingling in the hands and legs, difficulty walking, and nerves in the bladder or intestines being affected, leading to urinary incontinence, as well as severe pain when sitting or bending. As for the treatment of this disease, it includes several types, including: surgery, the use of muscle relaxants, the use of steroid injections, or non-steroidal anti-inflammatory drugs.
The location of spinal stenosis determines how it is classified. Doctors distinguish between two types of stenosis: stenosis in the neck or lower back, which is the most common. The ligaments or cords that hold the spine together may thicken and become harder with age, making this disease more common in men and women over the age of fifty. Bones and joints can also grow, narrowing the spaces between the vertebrae and causing arthritis, which becomes more common as you get older and can become more severe.
It can, however, happen in younger people who were born with spinal canal stenosis or who have had a spinal injury. Disc disease, in which the discs that separate the vertebrae crack and drop, can also be a cause. Tumors in the spine or a sudden exposure to an injury that results in a change in the spine or the emergence of bone fragments at the site of the injury are two other causes.
This condition results in muscle spasm, pain, or numbness in the legs, back, neck, shoulders or arms, sensory loss in the extremities, and sometimes bladder and bowel dysfunction.
Osteoporosis of the vertebrae
One of the most common diseases of the spine is osteoporosis of the vertebrae, which is caused by the bones losing their ability to withstand injuries and shocks, as well as a lack of bearing excessive body weight. Genetic factors, a lack of physical activity, a nutrient-deficient diet, as well as advancing age and hormonal imbalances, are all factors that contribute to the disease. This disease is treated with a combination of vitamin D and calcium-rich foods and hormonal drugs.
When the rate of new bone formation is slower than the rate of old bone decomposition, osteoporosis develops, and osteoporosis-related fractures develop in the hip, wrist, and spine.
The problem with osteoporosis of the spine is that it has no symptoms, and patients are unaware of their injury until after it has occurred. However, some symptoms, such as pain in the lower back, tingling from the bottom of the leg to the foot, and the inability to stand straight without pain, may indicate a problem with the bones.
Spinal tumors
Tumors that affect the vertebrae can spread from cancers in other parts of the body, but some tumors, such as chordoma, chondrosarcoma, osteosarcoma, plasmacytoma, and Ewing’s sarcoma, start within the bones of the spine. Spinal tumors can be cancerous or non-cancerous, and they can arise in the spine or spread from another part of the body to the vertebrae, which is known as secondary. About a third of primary myeloid tumors originate in cells within the spinal cord, and these tumors can extend within the spinal cord to block the flow of cerebrospinal fluid, resulting in the formation of a fluid-filled cavity -syrinx-, whereas the majority of primary spinal cord tumors originate in cells adjacent to the spinal cord, such as those in the meninges. Meningiomas and neurofibromas, which arise in cells adjacent to the medulla, are the most common benign, noncancerous tumors.
The most common type of myeloma tumor is secondary myeloma. They are cancerous metastases that originate in another part of the body and have spread to the vertebrae. These metastatic cancers put pressure on the spinal cord and nerve roots in the marrow, as well as invade and destroy bone.
The spinal cord, nerve roots, blood vessels, and bones of the spine are all affected by spinal tumors. Back pain is a common symptom of spinal tumors in the early stages. Hips, legs, feet, and arms may also be affected, and the pain may worsen over time. Because the tumor mass is growing, the patient may experience pain at the tumor site.
Back pain that spreads to other parts of the body and gets worse at night, difficulty walking, which can lead to falls and balancing problems; the patient also has loss of sensation or muscle weakness, particularly in the arms and legs. Muscle weakness in various parts of the body, which can be mild or severe.
To treat the tumor, neurosurgeons use ultrasound, microsurgery, and laser surgery, and modern fusion and stabilization techniques, such as vertebroplasty and meningectomy, help restore functional movement and relieve pain.
You can contact us via WhatsApp for any medical consultation. Also, you can discover more medical articles from our website.